At WiseGEEK, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is a Dehisced Wound?
A dehisced wound is a surgical wound that has opened up during the healing process. In some cases, wound dehiscence can be a medical emergency requiring immediate surgery to repair the wound. For less severe cases, it may be treated with careful bandaging and monitoring to check for signs of further dehiscence or infection. While people recover from surgery in the hospital, nurses check their healing wounds regularly for signs of complications like spontaneous ruptures and once they arrive home, people should keep an eye on their surgical wounds. If there are any signs of dehiscence, the surgeon should be called immediately.
There are a number of factors known to lead to spontaneous ruptures of surgical wounds. Abdominal surgeries are far more likely to end with a dehisced wound and these wounds can come with serious complications like evisceration, where the contents of the abdomen protrude out of the wound when it splits open. People with medical conditions like connective tissue disorders and diabetes are at increased risk of developing a dehisced wound. Sometimes, this surgical complication is the result of placing sutures incorrectly.

A major concern with spontaneous reopening of surgical wounds is the potential for infection. If a wound opens up, bacteria and other organisms can work their way into the surgical site and cause complications for the patient. The wound may also become inflamed and chronically irritated, making it difficult for the injury to heal or causing severe scarring when the wound does close. It is also possible for a dehisced wound to widen beyond the original boundaries of the surgical site as a result of tension on the edges of the wound.

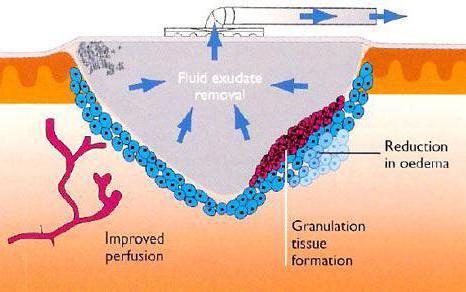
In a mild case, the surgical wound opens slightly, but does not rupture all along its length or all the way to the base of the incision. The surgeon should be called to examine the wound. Typically the wound is irrigated to remove any bacteria present and then it will be bandaged to protect it. More serious open wounds may be treated with a vacuum bandage to keep the wound closed and allow the edges to start knitting together.

In deep dehisced wounds or wounds where evisceration has occurred, the patient needs surgery. The bound will be covered with moist bandage material and the patient will be prepared for surgery. If a patient is too unstable for surgery, supportive care will be provided while hospital personnel work on stabilizing the patient for the operating room.
AS FEATURED ON:
AS FEATURED ON:













Discussion Comments
@ mabeT- Howdy! You really need to get that boy to sit down and take it easy. A wound reopening is not a fun thing in any way, shape or form.
Are you in a position to help him with the things that he feels are so important? Can you arrange for someone else to do so?
Explain to him that if he will just sit on his butt until the doctor says it is okay to get up, he will get well faster.
After a wound has opened back up, you’re back at square one, baby. Maybe you should look up some dehiscenece wound pictures for him to take a gander at! That's bound to get him back in the recliner!
Good luck with your stubborn man!
Is a patient at more risk of a dehiscence wound if they do not follow doctor recommendations about resting after a major surgery? It seems that this could be very serious indeed.
I have a friend who recently underwent a hernia operation, and he refuses to sit down and take it easy.
He has twelve (that’s right; count ‘em, twelve)staples on his side and thinks that housework and yard work is just too imminent for him to rest for a couple of weeks.
My mother had to have a double mastectomy some years ago, and she had reconstructive surgery with implants.
These did not work well for her, causing her a great deal of pain. So her doctor suggested that she do another type of reconstructive where the stomach muscles were clipped, pushed up diagonally and substituted for breasts.
This was a disaster. She had an incision that ran across the bottom of her entire abdomen, just above the pelvic area, from hip to hip. The doctor lost her on the table three times from blood loss, and he closed her up hurriedly.
This incision busted open time and again, and eventually could not be closed again because of rotting skin and flesh. She was like this for months, and in severe agony.
Once it did start to finally come together, she began to form hard spots under the skin of the scar which she said hurt and burned. We discovered that these were improperly placed staples once they began popping out of her skin, and reopening the wound in places.
Come to find out the doctor in question had never performed this surgery before, and was not qualified to do so.
The wound healing did not actually complete itself for over a year after the surgery.
Post your comments