At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is a Spinal Abscess?
A spinal abscess is a pus-filled cyst or lesion that develops in soft tissue surrounding the spinal cord. Most abscesses are formed in the lower or middle back due to infectious bacteria building up in the region. Many different types of bacteria can cause infection, and a spinal abscess may develop after pathogens enter a wound on the back or spread to the spine from another part of the body through the blood. Pain, swelling, fever, and chills are common, and more serious symptoms of paralysis and weakness can occur if an abscess compresses the spinal cord. Antibiotics and anti-inflammatory drugs can usually relieve symptoms, though a progressed abscess may need to be surgically drained.
Persistent strains of staphylococcus are the most common bacterial cause of a spinal abscess, though several other pathogens may be involved. Infection can enter the space around the spinal cord through a break in tissue from a traumatic injury or an unhealed surgical wound. Occasionally, bacteria makes their way to the spine from another infection site such as the throat or lungs.

The first symptoms of a spinal abscess may include a worsening backache, tenderness and swelling in the spine, and flu-like symptoms of fever, chills, and fatigue. Some people experience headaches, nausea, and vomiting as well. If a cyst grows large enough to put pressure on the spinal cord, an individual can lose feeling and motor movement ability in the legs, arms, or elsewhere in the body. Without treatment, a spinal abscess can lead to major paralysis.

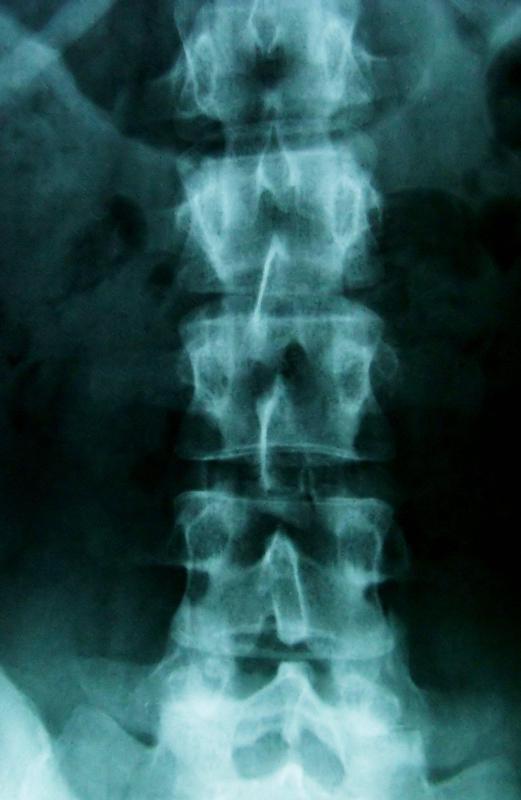
A doctor can usually diagnose a spinal abscess by reviewing symptoms and feeling the section of swollen back tissue. He or she may decide to perform computerized tomography scans and x-rays to confirm that an abscess exists and rule out other problems such as tumors, bone deformities, and slipped disks. A sample of blood or cerebrospinal fluid may be collected and cultured in a laboratory to determine the type of bacteria responsible for symptoms.

Treatment options can be discussed after the diagnosis is confirmed. Patients with relatively small abscesses and no symptoms of weakness or numbness can usually be treated on an outpatient basis with oral antibiotics. Mild pain and inflammation can be relieved with spinal corticosteroid injections. Most small abscesses and accompanying infections are resolved in four to six weeks.

If spinal cord compression exists, a patient is typically hospitalized and scheduled for immediate surgery. A specialist performs needle aspiration to drain pus from the spinal abscess and relieve spinal cord tension. Rarely, additional surgeries are needed to repair damaged tissue and realign vertebrae. Recovery can take several weeks or months depending on the type of surgery received, but most patients do eventually get better without lasting movement problems.
AS FEATURED ON:
AS FEATURED ON:
















Discuss this Article
Post your comments