At TheHealthBoard, we're committed to delivering accurate, trustworthy information. Our expert-authored content is rigorously fact-checked and sourced from credible authorities. Discover how we uphold the highest standards in providing you with reliable knowledge.
What is Mucous Colitis?
Mucous colitis is a gastrointestinal symptom characterized by inflammation of the intestines and subsequent overproduction of mucus. The patient experiences irregular bowel movements that can alternate between diarrhea and constipation and are typically slimy as a result of the large amounts of mucus being passed in the stool. A number of conditions can be associated with mucous colitis and proper treatment requires a diagnostic evaluation to learn more about what is happening inside the patient's bowels.
Crohn's disease, ulcerative colitis, anal fissures, irritable bowel syndrome, bowel obstructions, and bowel infections are all associated with mucus colitis. In all cases, the bowel becomes inflamed and the cells that line the bowel produce more mucus than usual in response. Commonly, intestinal motility increases, causing pain and cramping, as well as interfering with digestion. In some cases, fresh blood can be observed in the stool.

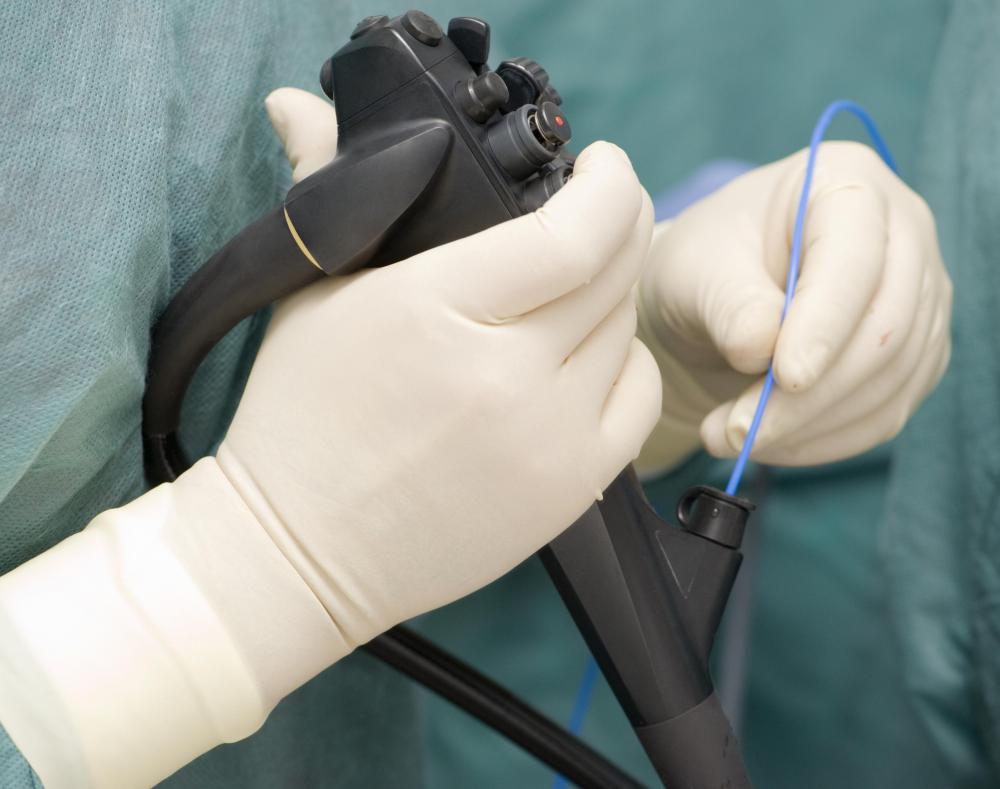
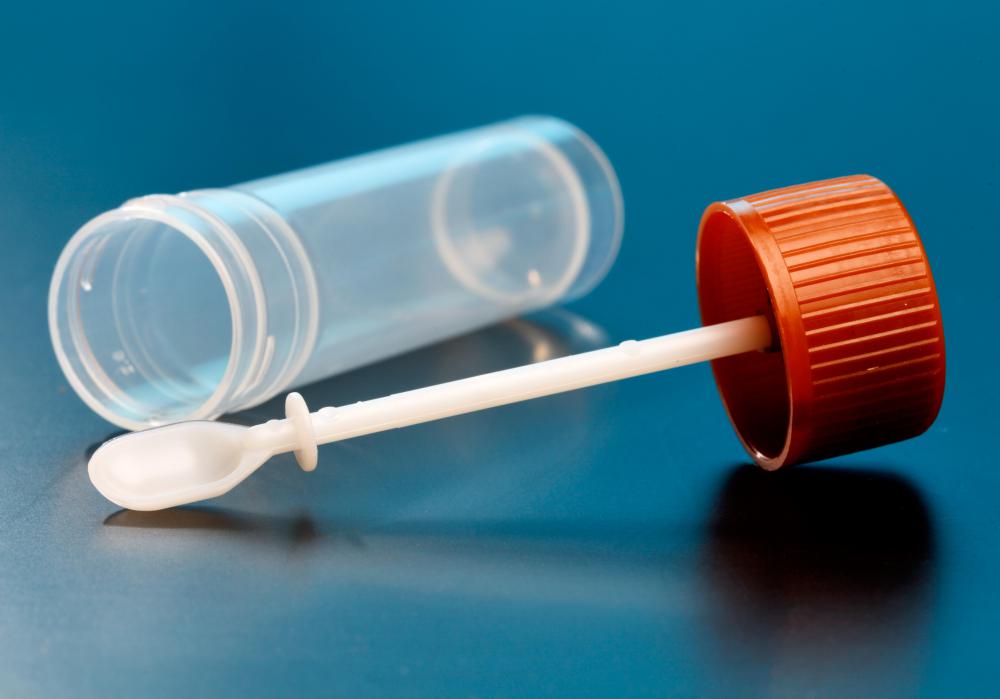
When a patient presents with mucous colitis, stool samples are often examined to look for causative agents like infectious bacteria in the bowel. Other diagnostic techniques can include endoscopy, the use of a camera to look inside the bowels, along with bowel biopsy, and exploratory surgery. Diagnostic material is collected and evaluated to narrow down a cause for the colitis. To keep the patient comfortable, bowel protectants may be prescribed along with anti-inflammatory medications.

Treatment options vary, depending on why a patient has mucous colitis. Sometimes, medications can be used to control an underlying health problem. Dietary adjustments may also help, and in some cases, patients may benefit from therapy to address anxiety disorders and other mental health disorders, as this condition can be associated with psychological distress at times. In some cases, surgery may be necessary to treat areas of extreme inflammation.

Mucous colitis can be recurrent and over time, the treatment regimen may need to be adjusted. People can develop flareups followed by long intervals of relatively good health. Learning to recognize triggers associated with onset can help people avoid future episodes. Potential triggers can vary, depending on the underlying cause, but can be related to diet, stress, and general health. Common dietary triggers include greasy or especially spicy food.

People with this condition are at increased risk of developing intestinal cancers, as the chronic irritation increases the rate of cell division and can permit cancerous cells to develop. People with a history of mucous colitis and other forms of bowel inflammation should be regularly screened for cancer. Intestinal cancers are much easier to treat when caught early and the complications associated with cancer treatment can be significantly reduced with early diagnosis and treatment.
AS FEATURED ON:
AS FEATURED ON:















Discussion Comments
Ugh. That condition is, indeed, one of the fun filled bonuses of ulcerative colitis. Anyone having this condition regularly should have it checked out as ulcerative colitis and Chron's disease both have to be monitored regularly because they can be a primary factor in the development of colon cancer.
Post your comments